Globally, in 2017, there were ~41.2 million prevalent cases of gout, with 7.4 million incident cases per year adding up to almost 1.3 million years lived with disability.1 In the U.S., approximately 3.9% (9.2 million) of Americans have a history of gout, but men (5.2%, 5.9 million) are much more likely to report having this disease than women (2.7%, 3.3 million).2
Gout is the most common form of inflammatory arthritis worldwide. It is caused by deposition of monosodium urate crystals in joints and various other tissues and appears in relation to chronic hyperuricemia.3 Definitions of hyperuricemia vary, but Bardin and Richette4 proposed defining hyperuricemia as serum uric acid (SUA) levels above 6mg/dl, based on the increased life-long risk for developing gout that starts at this level. Elevated uric acid levels may also be a risk factor for cardiovascular disease (CVD).5
Uric acid is the final enzymatic product in the degradation of purine nucleosides and free bases in humans. It is produced by the conversion of the purine derivative hypoxanthine to xanthine and xanthine to uric acid by xanthine oxidase. Of the 4 purine bases, adenine and hypoxanthine are thought to have much more of an effect on uric acid levels than guanine and xanthine.6 More than 90% of gout patients have hyperuricemia; however, 90% of people with hyperuricemia remain asymptomatic.7,8
Traditionally, dietary recommendations related to gout have focused on limiting purine intake.9 For example, the 2017 position of the British Society for Rheumatology is that high purine foods should be avoided,10 and the 2014 Japanese Guidelines for the Management of Hyperuricemia and Gout recommend consuming less than 400mg of purines per day.11 However, there is debate about the value of restricting purine intake. According to Beyl and colleagues,12 the importance of patients with gout maintaining a low-purine diet has been deemphasized in recent years. And after reviewing nutritional recommendations for gout, Nielsen et al.13 concluded in 2018 that evidence in support of most of the dietary guidelines related to gout issued by health organizations/authorities are considered to be “moderate or low” or “very low” quality.
Recent results of a cross-sectional study involving more than 6,000 elderly participants of the PREDIMED-Plus study are relevant to the discussion about purine restriction.14 Despite consuming purine-rich foods (Table 1), individuals in the highest tertile of total non-soy legume, lentil, and pea consumption had statistically significantly lower SUA levels than those in the lowest tertile, whereas chickpea and dry bean intake was unrelated to uric acid levels. This finding may be because purine bases and metabolites involved in the endogenous synthesis of purines affect SUA levels differently.15 For this reason, dietary recommendations should not be based solely on the purine content of a food but also on how that food affects plasma urate.9
Despite age-standardized incidence rates of gout in South Asia, Southeast Asia, and East Asia being lower than in Western Europe and North America (Table 2), there is a common belief among health professionals in Asia that soyfoods increase risk of gout.16 This perspective conflicts with the position of the British Society for Rheumatology, which recommends the consumption of soybeans be encouraged in overweight patients with gout. Additionally, a meta-analysis by Li et al.17 found that soyfoods were inversely related to the risk of gout and hyperuricemia. However, these findings were based on only 2 studies, a cross-sectional study from Shanghai18 and a prospective study from Singapore.19
The Shanghai study involved 3,978 men aged 40-74. Hyperuricemia was defined as a blood uric acid level >7.0mg/dl. One quarter of this population had hyperuricemia. Dietary information was collected by using a food frequency questionnaire (FFQ). An inverse association between soyfood consumption and hyperuricemia was observed after adjustment for 14 potential confounders (odds ratios for quintiles 1-5: 1.00, 0.90, 0.70, 0.89, and 0.77).18 During the years 1993-1998, the cohort study from Singapore involved 63,257 adults between the ages of 45 and 74 at the time of recruitment. Habitual diet information was collected via a validated semiquantitative FFQ, and physician-diagnosed gout was self-reported during 2 follow-up interviews up to the year 2010. A total of 2,167 participants developed gout during the follow-up period. The multivariate-adjusted hazard ratio (95% confidence interval) of gout, comparing the fourth soyfood intake quartile with the first quartile, was 0.86 (0.75-0.98; P for trend = 0.018).19
Observational studies showing that SUA levels of vegetarians (for whom soy is typically a part of the diet) are similar to or lower than the SUA levels of non-vegetarians are of potential relevance to assessing the impact of soy intake on gout risk. These studies have been conducted in Taiwan,20-24 Hong Kong,25 and the United Kingdom.26 Urinary uric acid levels were also found to be reduced in response to a vegetarian diet, compared to a non-vegetarian diet.27,28 However, the informative value of this research as it relates to soy is limited because multiple lifestyle and dietary factors impact SUA acid levels (see next article).
In addition to the observational data, 7 intervention trials evaluating the effects of soy or a diet containing soy on uric acid levels were identified (Table 3). These studies varied in design, and all but one were acute studies meaning that changes in SUA levels were determined 1-4 hours after ingestion of a soy product. Breslau et al.29 reported there were no differences in SUA levels between a vegetarian and non-vegetarian diet after 9-12 days of following the respective diets. The exact amount of soy in the vegetarian diet was not indicated, but soymilk and 2 servings of textured vegetable (soy) protein were consumed daily. In contrast, Garell et al.30 found that SUA levels significantly increased by about 10% at 3 hours following ingestion of soy protein isolate; whereas levels decreased in response to casein and lactalbumin. Similar findings were reported by Dalbeth et al.31 However, the practical implications of this research are unclear because participants in these studies consumed 80g of each protein. Somewhat parenthetically, some evidence suggests that cow’s milk, as well as several other foods, may have a uricosuric effect.32
In the study by Brule et al.,33 SUA levels increased in 1 of 3 participant groups at 2 hours post soy ingestion, whereas there were increases in all 3 groups in response to haddock but no increase was observed in response to liver. Each of the varying protein sources provided 50g protein. The results of one study suggest different soyfoods affect SUA levels differently. In comparison to baseline, whole soybeans, soymilk, and soy powder led to a significant increase in SUA levels of approximately 5-10% at 1 and 2 hours post ingestion, but at 3 hours only the response to soymilk was significant. Furthermore, tofu did not cause an increase.34 However, not only was a non-soy protein control absent from this study, but the test products provided 40g protein, a much larger amount than would typically be consumed at one sitting.
The Japanese study by Yamashita et al.,35 which involved 8 heathy males and 10 males with gout, found that 4 hours post tofu ingestion, SUA levels increased from 5.56 to 5.73mg/dl in the former and increased from 8.10 to 8.12mg/dl in the latter. Assuming the participants weighed 70kg, they consumed approximately 17g soy protein from tofu. The authors concluded that the results suggest tofu is a preferable source of protein for gout patients. Finally, the consumption of soymilk that provided 15.5g protein also had no effect on SUA levels; however, the assessment was done only at 1-hour post-ingestion.
In summary, the limited observational data do not suggest soyfoods increases risk of gout or elevate SUA levels. One longer-term clinical trial shows soyfoods do not increase SUA levels. Several acute intervention studies show modest increases in SUA levels in response to soy protein, but the practical implications of this research are unclear given the large amounts of soy protein consumed (³40g) and when considering that studies intervening 15-17g soy protein showed no effect.
Finally, as noted at the onset, elevated SUA levels may be a risk factor for CVD.5 However, elevated SUA levels may impact more than gout and CVD. After extensively reviewing the literature, Kanbaya et al.36 concluded that uric acid is now being viewed “as a potential master conductor in the worldwide symphony of obesity, diabetes, and cardiorenal disease.” Given that the consumption of soyfoods at levels even higher than typically consumed by native Japanese37does not appear to increase SUA levels and that to varying degrees the evidence suggests that soyfoods may help to reduce risk of CVD38-41 and diabetes,42,43 it is reasonable to suggest that patients with gout consider adding soyfoods to their diet.
Table 1. Purine content of selected food groups and foods (mg/100g wet weight, edible portion) add more foods
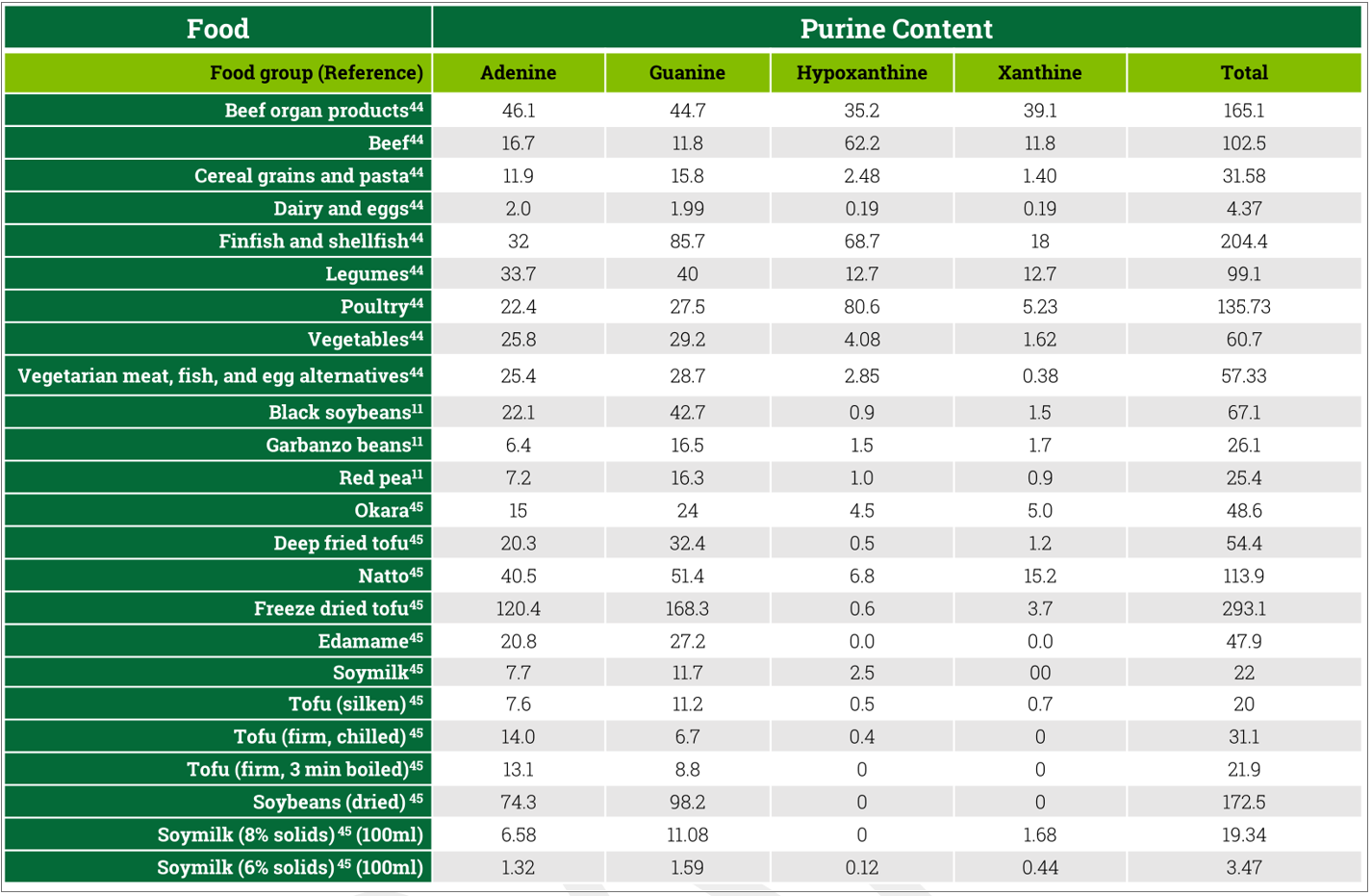
Table 2. Age-standardized incidence rates (per 100,00 population)46
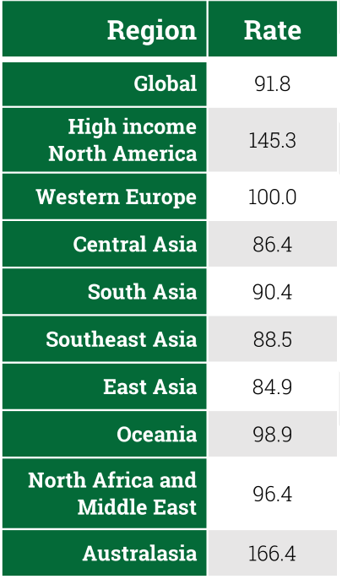
Table 3. Acute (3-4 hour) clinical studies examining the effect of soy protein on serum uric acid (SUA) and/or urinary uric acid (UUA) levels
Want to learn more? Download our full Gout and Soyfoods brochure
REFERENCES:
- Safiri S, Kolahi AA, Cross M, Carson-Chahhoud K, Hoy D, Almasi-Hashiani A, Sepidarkish M, Ashrafi-Asgarabad A, Moradi-Lakeh M, Mansournia MA, et al. Prevalence, incidence, and years lived with disability due to gout and its attributable risk factors for 195 countries and territories 1990-2017: A systematic analysis of the Global Burden of Disease Study 2017. Arthritis Rheumatol 2020;72:1916-27.
- Chen-Xu M, Yokose C, Rai SK, Pillinger MH, Choi HK. Contemporary prevalence of gout and hyperuricemia in the United States and decadal trends: The National Health and Nutrition Examination Survey, 2007-2016. Arthritis Rheumatol 2019;71:991-9.
- Kuo CF, Grainge MJ, Zhang W, Doherty M. Global epidemiology of gout: prevalence, incidence and risk factors. Nat Rev Rheumatol 2015;11:649-62.
- Bardin T, Richette P. Definition of hyperuricemia and gouty conditions. Curr Opin Rheumatol 2014;26:186-91.
- Yu W, Cheng JD. Uric acid and cardiovascular disease: An update from molecular mechanism to clinical perspective. Front Pharmacol 2020;11:582680.
- Sarwar G, Brule D. Assessment of the uricogenic potential of processed foods based on the nature and quantity of dietary purines. Prog Food Nutr Sci 1991;15:159-81.
- Eggebeen AT. Gout: an update. Am Fam Physician 2007;76:801-8.
- Vitart V, Rudan I, Hayward C, Gray NK, Floyd J, Palmer CN, Knott SA, Kolcic I, Polasek O, Graessler J, et al. SLC2A9 is a newly identified urate transporter influencing serum urate concentration, urate excretion and gout. Nat Genet 2008;40:437-42.
- Zgaga L, Theodoratou E, Kyle J, Farrington SM, Agakov F, Tenesa A, Walker M, McNeill G, Wright AF, Rudan I, et al. The association of dietary intake of purine-rich vegetables, sugar-sweetened beverages and dairy with plasma urate, in a cross-sectional study. PloS one 2012;7:e38123.
- Hui M, Carr A, Cameron S, Davenport G, Doherty M, Forrester H, Jenkins W, Jordan KM, Mallen CD, McDonald TM, et al. The British Society for Rheumatology Guideline for the Management of Gout. Rheumatology (Oxford) 2017;56:1246.
- Kaneko K, Takayanagi F, Fukuuchi T, Yamaoka N, Yasuda M, Mawatari KI, Fujimori S. Determination of total purine and purine base content of 80 food products to aid nutritional therapy for gout and hyperuricemia. Nucleosides Nucleotides Nucleic Acids 2020;39:1449-57.
- Beyl RN, Jr., Hughes L, Morgan S. Update on importance of diet in gout. Am J Med 2016;129:1153-8.
- Nielsen SM, Zobbe K, Kristensen LE, Christensen R. Nutritional recommendations for gout: An update from clinical epidemiology. Autoimmun Rev 2018;17:1090-6.
- Becerra-Tomas N, Mena-Sanchez G, Diaz-Lopez A, Martinez-Gonzalez MA, Babio N, Corella D, Freixer G, Romaguera D, Vioque J, Alonso-Gomez AM, et al. Cross-sectional association between non-soy legume consumption, serum uric acid and hyperuricemia: the PREDIMED-Plus study. Eur J Nutr 2020;59:2195-206.
- Clifford AJ, Riumallo JA, Young VR, Scrimshaw AS. Effect of oral purines on serum and urinary uric acid of normal, hyperuricemic and gouty humans. J Nutr 1976;106:428-34.
- Messina M, Messina VL, Chan P. Soyfoods, hyperuricemia and gout: A review of the epidemiologic and clinical data. Asia Pacific journal of clinical nutrition 2011;20:347-58.
- Li R, Yu K, Li C. Dietary factors and risk of gout and hyperuricemia: a meta-analysis and systematic review. Asia Pacific journal of clinical nutrition 2018;27:1344-56.
- Villegas R, Xiang YB, Elasy T, Xu WH, Cai H, Cai Q, Linton MF, Fazio S, Zheng W, Shu XO. Purine-rich foods, protein intake, and the prevalence of hyperuricemia: the Shanghai Men's Health Study. Nutrition, metabolism, and cardiovascular diseases : NMCD 2012;22:409-16.
- Teng GG, Pan A, Yuan JM, Koh WP. Food sources of protein and risk of incident gout in the Singapore Chinese Health Study. Arthritis Rheumatol 2015;67:1933-42.
- Pan WH, Chin CJ, Sheu CT, Lee MH. Hemostatic factors and blood lipids in young Buddhist vegetarians and omnivores. Am J Clin Nutr 1993;58:354-9.
- Chen CW, Lin CT, Lin YL, Lin TK, Lin CL. Taiwanese female vegetarians have lower lipoprotein-associated phospholipase A2 compared with omnivores. Yonsei Med J 2011;52:13-9.
- Kuo CS, Lai NS, Ho LT, Lin CL. Insulin sensitivity in Chinese ovo-lactovegetarians compared with omnivores. Eur J Clin Nutr 2004;58:312-6.
- Chiu THT, Liu CH, Chang CC, Lin MN, Lin CL. Vegetarian diet and risk of gout in two separate prospective cohort studies. Clin Nutr 2020;39:837-44.
- Lin CK, Lin DJ, Yen CH, Chen SC, Chen CC, Wang TY, Chou MC, Chang HR, Lee MC. Comparison of renal function and other health outcomes in vegetarians versus omnivores in Taiwan. J Health Popul Nutr 2010;28:470-5.
- Szeto YT, Kwok TC, Benzie IF. Effects of a long-term vegetarian diet on biomarkers of antioxidant status and cardiovascular disease risk. Nutrition 2004;20:863-6.
- Schmidt JA, Crowe FL, Appleby PN, Key TJ, Travis RC. Serum uric acid concentrations in meat eaters, fish eaters, vegetarians and vegans: A cross-sectional analysis in the EPIC-Oxford cohort. PloS one 2013;8:e56339.
- Siener R, Hesse A. The effect of different diets on urine composition and the risk of calcium oxalate crystallisation in healthy subjects. Eur Urol 2002;42:289-96.
- Siener R, Hesse A. The effect of a vegetarian and different omnivorous diets on urinary risk factors for uric acid stone formation. Eur J Nutr 2003;42:332-7.
- Breslau NA, Brinkley L, Hill KD, Pak CY. Relationship of animal protein-rich diet to kidney stone formation and calcium metabolism. J Clin Endocrinol Metab 1988;66:140-6.
- Garrel DR, Verdy M, PetitClerc C, Martin C, Brule D, Hamet P. Milk- and soy-protein ingestion: acute effect on serum uric acid concentration. Am J Clin Nutr 1991;53:665-9.
- Dalbeth N, Wong S, Gamble GD, Horne A, Mason B, Pool B, Fairbanks L, McQueen FM, Cornish J, Reid IR, et al. Acute effect of milk on serum urate concentrations: a randomised controlled crossover trial. Ann Rheum Dis 2010;69:1677-82.
- Towiwat P, Li ZG. The association of vitamin C, alcohol, coffee, tea, milk and yogurt with uric acid and gout. Int J Rheum Dis 2015;18:495-501.
- Brule D, Sarwar G, Savoie L. Changes in serum and urinary uric acid levels in normal human subjects fed purine-rich foods containing different amounts of adenine and hypoxanthine. J Am Coll Nutr 1992;11:353-8.
- Zhang M, Lin L, Liu H. Acute effect of soy and soy products on serum uric acid concentration among healthy Chinese men. Asia Pacific journal of clinical nutrition 2018;27:1239-42.
- Yamakita J, Yamamoto T, Moriwaki Y, Takahashi S, Tsutsumi Z, Higashino K. Effect of Tofu (bean curd) ingestion and on uric acid metabolism in healthy and gouty subjects. Adv Exp Med Biol 1998;431:839-42.
- Kanbay M, Jensen T, Solak Y, Le M, Roncal-Jimenez C, Rivard C, Lanaspa MA, Nakagawa T, Johnson RJ. Uric acid in metabolic syndrome: From an innocent bystander to a central player. European journal of internal medicine 2016;29:3-8.
- Messina M, Nagata C, Wu AH. Estimated Asian adult soy protein and isoflavone intakes. Nutr Cancer 2006;55:1-12.
- Xue T, Wen J, Wan Q, Qin G, Yan L, Wang G, Qin Y, Luo Z, Tang X, Huo Y, et al. Association of soy food with cardiovascular outcomes and all-cause mortality in a Chinese population: a nationwide prospective cohort study. Eur J Nutr 2022;61:1609-20.
- Wang X, Yu C, Lv J, Li L, Hu Y, Liu K, Shirai K, Iso H, Dong JY. Consumption of soy products and cardiovascular mortality in people with and without cardiovascular disease: a prospective cohort study of 0.5 million individuals. Eur J Nutr 2021;60:4429-38.
- Blanco Mejia S, Messina M, Li SS, Viguiliouk E, Chiavaroli L, Khan TA, Srichaikul K, Mirrahimi A, Sievenpiper JL, Kris-Etherton P, et al. A meta-analysis of 46 studies identified by the FDA demonstrates that soy protein decreases circulating LDL and total cholesterol concentrations in adults. J Nutr 2019;149:968-81.
- Jenkins DJA, Blanco Mejia S, Chiavaroli L, Viguiliouk E, Li SS, Kendall CWC, Vuksan V, Sievenpiper JL. Cumulative meta-analysis of the soy effect over time. Journal of the American Heart Association 2019;8:e012458.
- Jain R, Bolch C, Al-Nakkash L, Sweazea KL. Systematic review of the impact of genistein on diabetes related outcomes. Am J Physiol Regul Integr Comp Physiol 2022.
- Baranska A, Blaszczuk A, Polz-Dacewicz M, Kanadys W, Malm M, Janiszewska M, Jedrych M. Effects of soy isoflavones on glycemic control and lipid profile in patients with Type 2 Diabetes: A systematic review and meta-analysis of randomized controlled trials. Nutrients 2021;13.
- Wu B, Roseland JM, Haytowitz DB, Pehrssonb PR, Ershow AG. Availability and quality of published data on the purine content of foods, alcoholic beverages, and dietary supplements. J Food Comp Anal 2019;84:103281.
- Fukuuchi T, Itahashi I, Takayanagi F, Yamaoka N, Kaneko K. Determination of total purine and free purine content in milk, soymilk, and enteral nutritional supplements to assist nutritional therapy for hyperuricemia and gout. Nucleosides Nucleotides Nucleic Acids 2022:1-9.
- Safiri S, Kolahi A A, Cross M, Carson-Chahhoud K, Hoy D, Almasi-Hashiani A, Sepidarkish M, Ashrafi-Asgarabad A, Moradi-Lakeh M, Mansournia M A, et al.; Prevalence, incidence, and years lived with disability due to gout and its attributable risk factors for 195 countries and territories 1990-2017: A systematic analysis of the Global Burden of Disease Study 2017. Arthritis Rheumatol. (2020) 72:1916-1927.
- Serrano JC, Martin-Gari M, Cassanye A, Granado-Serrano AB, Portero-Otin M. Characterization of the post-prandial insulinemic response and low glycaemic index of a soy beverage. PloS one 2017;12:e0182762.
